
Introduction
Healthcare providers and payers are trapped in a prior authorization crisis. Manual review processes create multi-day delays that affect patient care, fuel physician burnout, and drain administrative budgets. According to the AMA's 2024 survey of 1,000 practicing physicians, physicians and staff spend 13 hours per week on prior authorization tasks alone—time taken directly away from patient care.
AI's most measurable impact in healthcare isn't in diagnostics or drug discovery—it's in prior authorization. When approvals stall, patients abandon treatments, clinical outcomes suffer, and administrative costs climb as payer requirements grow more complex.
This article breaks down how AI in prior authorization delivers concrete operational results: faster approvals, lower administrative overhead, and compliance that keeps pace with evolving payer rules.
TL;DR
- AI automates documentation gathering, eligibility checks, and form submission—replacing processes that take days with ones that take minutes
- Faster approvals, fewer staff hours on manual tasks, and fewer denials from incomplete documentation follow directly
- Healthcare organizations report lower operational costs, less physician burnout, and stronger care continuity for patients
- CMS regulations effective 2026 mandate faster prior authorization decisions—AI adoption is now a compliance requirement, not just an efficiency play
- EHR integration and human clinical oversight multiply these gains across the full authorization workflow
What Is AI in Prior Authorization?
AI in prior authorization is the use of machine learning, natural language processing, and automation to handle the steps required to obtain insurance approval before delivering a medical service. This includes pulling clinical records, checking payer criteria, auto-populating payer forms, and submitting requests.
Where it's applied:
- Hospitals and health systems
- Specialty practices (oncology, radiology, cardiology, pharmacy)
- Payer organizations
- Insurance companies
In practice, AI triggers automatically at point-of-care ordering within EHR systems — the moment a physician places an order, the authorization process begins in the background. It operates across multiple specialties and handles administrative steps that carry no clinical value, freeing clinicians and staff to focus on patient care.
Clinical judgment remains central to the process. AI handles the documentation and routing work; physicians and care teams retain oversight for complex or edge-case decisions where context matters.
Key Advantages of AI in Prior Authorization
Each advantage below maps directly to a metric healthcare finance, operations, or clinical leaders track: turnaround time, staff hours, cost per request, denial rates, and patient outcomes.
Advantage 1: Faster Approval Turnaround
AI systems detect when prior authorization is required, gather documentation, and submit a complete request to the payer in minutes—no waiting for staff availability or manual form completion.
By integrating with EHR systems, AI agents automatically pull:
- Structured clinical data (diagnosis codes, treatment history, coverage details)
- Unstructured documents (clinical notes, imaging reports)
AI then maps this data against payer-specific criteria in real time, completing the authorization without human intervention at each step.
Delays in prior authorization directly delay patient care. The AMA's 2024 survey found that 93% of physicians report prior authorization delays access to necessary care, and 82% report these delays can lead to treatment abandonment. For time-sensitive diagnoses—oncology, cardiovascular events—the gap between days and minutes is a patient safety issue, not just an operational one.
CMS now requires federally regulated health plans to complete standard prior authorization decisions within 7 calendar days. AI directly enables this compliance requirement.
KPIs impacted: authorization turnaround time, on-time submission rate, patient appointment rescheduling frequency, CMS mandate compliance.
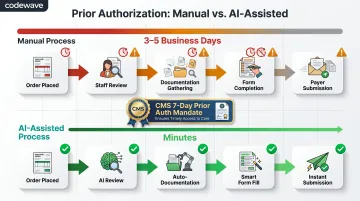
This advantage matters most for:
- High-volume specialty practices
- Health systems operating across complex multi-payer environments
- Organizations subject to CMS Medicare Advantage or Medicaid regulations
Advantage 2: Reduced Administrative Burden and Operational Costs
AI takes over the most time-intensive administrative tasks—documentation collection, form filling, payer portal navigation, and status follow-up—freeing staff to focus on higher-value work.
Instead of staff manually gathering records from multiple systems, AI agents run these steps in parallel across payers, handling form variations and documentation standards without dedicated staff time per request.
The AMA's 2024 survey shows physicians and staff spend 13 hours per week on prior authorization tasks—a direct driver of labor cost and burnout. 40% of physician offices employ staff whose primary role is prior authorization management. AI restructures this cost model.
The financial case is clear:
| Cost Metric | Manual | Electronic | Savings |
|---|---|---|---|
| Provider cost per transaction | $10.97 | $5.79 | $5.18 |
| System-wide savings opportunity | — | — | $515M/year |

Health Affairs estimates each transaction costs practices $20–$30 and payers $40–$50, putting total annual system cost at $35 billion.
KPIs impacted: staff hours per request, cost per authorization, FTE allocation to admin tasks, appeal rate, physician burnout scores.
This advantage matters most for:
- Multi-specialty groups processing thousands of authorizations per month
- Organizations experiencing staffing shortages
- Health systems looking to scale without proportional headcount growth
Speed and cost savings compound when accuracy improves. Fewer errors mean fewer denials—and fewer denials mean fewer appeals consuming the staff hours AI just freed up.
Advantage 3: Higher Accuracy, Fewer Denials, and Better Compliance
AI reduces denials caused by incomplete or mismatched documentation by ensuring every submission includes the precise clinical evidence each payer requires—before the request is sent.
By training on payer-specific medical necessity criteria and clinical guidelines, AI models can:
- Flag missing documentation before submission
- Identify mismatches between diagnosis codes and requested services
- Validate that submissions meet approval criteria
These are the errors human staff under time pressure routinely miss.
KFF's analysis of 2024 Medicare Advantage data shows 7.7% of 52.8 million prior authorization determinations were fully or partially denied. Only 11.5% of those denials were appealed—yet 80.7% of appealed denials were overturned. That overturn rate signals that most initial denials stem from documentation errors or incomplete submissions, not clinical inappropriateness. They were avoidable.
Each denied request triggers an appeal cycle that consumes staff time and delays care further. AI that catches errors upfront breaks this loop.
Starting March 2026, CMS requires health plans to publicly report denial rates, appeal rates, and overturn rates. AI that produces consistent, defensible decisions supports this compliance requirement directly.
KPIs impacted: first-pass approval rate, denial rate by cause, appeal volume and success rate, documentation completeness score, payer audit readiness.
This advantage matters most for:
- Organizations operating across multiple payer contracts with varying criteria
- Specialty practices with high denial rates in specific service lines
- Payers or health plans subject to CMS reporting mandates
What Happens When AI Is Absent from Prior Authorization
Without AI, staff spend the equivalent of nearly two business days per week per physician on prior authorization tasks. This time is pulled directly from patient care and is a leading driver of physician burnout. AMA's 2024 survey found that 89% of physicians report prior authorization somewhat or significantly increases burnout.
Downstream consequences of continued manual processing:
- Inconsistent submissions drive higher denial rates and costly appeals cycles
- Treatment delays push patients to abandon recommended care; AMA data shows 29% of physicians reported prior authorization led to a serious adverse event — including hospitalization, permanent impairment, or death
- Administrative costs climb as authorization volume grows: KFF reports prior authorization requests per Medicare Advantage enrollee rose from 1.4 in 2020 to 1.7 in 2024
- Scaling becomes impossible without hiring: MGMA's 2026 Regulatory Burden Report found 92% of practices hired or reallocated staff specifically to handle prior authorizations

Regulatory risk:
Without AI-assisted automation, health plans face significant difficulty meeting the CMS 7-day turnaround mandate and the upcoming public reporting requirements, exposing them to financial penalties and reputational damage.
How to Get the Most Value from AI in Prior Authorization
Organizations seeing the strongest results from AI in prior authorization share a few common implementation practices—tool adoption alone doesn't guarantee them.
Integrate at the point of care:
AI works best when embedded directly inside EHR workflows—triggering automatically when an order is placed rather than requiring staff to initiate a separate process. EHR integration determines whether adoption is sustained or abandoned.
The CMS Interoperability and Prior Authorization Final Rule mandates that impacted payers implement a Prior Authorization API by January 1, 2027, reinforcing the regulatory push toward API-based workflows that connect directly with EHR ordering.
Maintain clinical oversight as a design principle:
The greatest risk of AI in prior authorization is removing human judgment entirely. Effective implementations use AI to handle administrative steps and flag edge cases for human review—not to make clinical necessity decisions autonomously. This protects organizations from regulatory and liability exposure.
Physicians are rightly concerned about AI systems that enable "systematic batch denials" without clinical review. The key safeguard is ensuring human clinical oversight is preserved in any AI-assisted authorization workflow.
Review outcomes continuously:
Track performance against concrete operational metrics to catch drift before it affects approval rates or patient care:
- First-pass approval rates by payer and service line
- Turnaround time from request submission to decision
- Denial trends and the clinical rationale behind them
- Staff time per authorization request
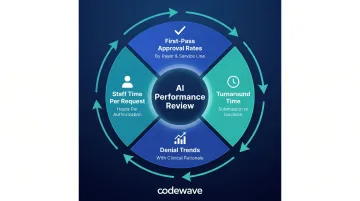
AI performance must be monitored regularly and the model updated as payer criteria evolve—what worked six months ago may not reflect current plan rules.
Implementation partners like Codewave structure this through Codewave's ImpactIndex™ model—tying development milestones directly to operational KPIs like approval rate improvement and turnaround reduction, so refinements are driven by real performance data rather than deployment schedules.
Conclusion
AI in prior authorization's core value is measurable and compounding: faster decisions, lower per-submission costs, and more accurate clinical documentation — each one amplifying the others as payer complexity increases.
That compounding effect only holds when AI is applied consistently across payer types, reviewed against real outcome data, and maintained as an evolving system — not deployed once and forgotten.
As CMS mandates tighten and administrative costs rise, the question shifts from whether to adopt AI in prior authorization to how quickly organizations can implement it effectively. Those that invest now in EHR integration, clinical oversight, and continuous performance monitoring will be able to grow patient volume without adding proportional administrative headcount.
Frequently Asked Questions
Can AI do prior authorizations?
Yes, AI can handle multiple steps of the prior authorization process—including detecting when authorization is needed, gathering clinical documentation, completing payer-specific forms, and submitting requests—typically reducing processing time from days to minutes. Clinical oversight remains necessary for complex or edge-case decisions.
Are there HIPAA-compliant AI tools for healthcare?
Yes, and they're increasingly standard. Before implementation, verify SOC 2 Type II certification, HITRUST compliance, and data handling practices, as required by the HHS HIPAA Security Rule. Responsible vendors build audit-ready workflows and access controls in by default.
How long does AI-assisted prior authorization take compared to manual processing?
Manual prior authorization typically takes one to several business days per request, while AI-assisted systems can process and submit a complete authorization request in minutes. Actual turnaround still depends on payer response times, but complete and accurate submissions consistently receive faster decisions.
Does AI in prior authorization reduce claim denials?
Well-implemented AI reduces denials caused by documentation errors, missing information, or payer criteria mismatches—which account for a significant portion of initial denials. AI validates submissions against payer-specific criteria before sending, catching gaps that manual processes frequently miss under time pressure.
What are the risks of using AI for prior authorization?
The primary risk lies in how AI is deployed. Payer-side AI used to batch-deny claims without clinical review has raised serious concerns from physician groups. Any AI-assisted workflow should preserve human clinical oversight as a non-negotiable safeguard.
How does AI in prior authorization integrate with existing EHR systems?
AI prior authorization tools typically integrate via API connections or native EHR marketplace apps (such as Epic's App Orchard), triggering automatically when a clinician enters an order that requires authorization. Successful integration means staff never leave their existing workflow—no system switching, no duplicate data entry, and no additional training burden for clinical teams.


