
Introduction
Healthcare organizations face a critical inefficiency crisis: physicians average 59-hour workweeks, with over 20% spending more than 8 hours weekly on after-hours EHR work — time that could otherwise go toward direct patient care. Administrative burdens consume roughly one-quarter of nearly $4 trillion in annual U.S. healthcare spending, representing up to $265 billion in potential savings through administrative simplification and automation. The global RPA in healthcare market hit $1.9 billion in 2023 and is projected to reach $9.5 billion by 2030 — a 25.9% annual growth rate that reflects how quickly the industry is responding.
Robotic Process Automation (RPA) offers a proven path to reclaim this lost capacity. This article covers what RPA is, where it delivers measurable value in healthcare, the challenges organizations encounter, and how to start building a business case.
TLDR:
- RPA automates rules-based tasks — claims, scheduling, data entry — without replacing existing systems
- High-impact use cases: claims processing, prior authorization, EHR data management, and scheduling
- Organizations report up to 69% cost reduction and 70% faster processing times
- Key challenges: data security, staff resistance, and upfront implementation complexity
- Start with high-volume, low-complexity processes to prove ROI quickly
What Is RPA in Healthcare?
Robotic Process Automation (RPA) refers to software bots that emulate human processes by combining APIs and user interface interactions to execute repetitive, rule-based tasks at scale. Unlike traditional automation that requires system-level integration or backend changes, RPA operates non-invasively — working on top of existing interfaces just as a human user would.
Why Healthcare Is Ideal for RPA
Healthcare operates under uniquely demanding conditions: high transaction volumes, complex compliance protocols, strict billing codes, and constantly shifting insurance rules. These workflows are often:
- Repetitive across thousands of patient interactions
- Rule-driven with clear decision trees
- Fragmented across multiple legacy systems
- Time-sensitive, affecting patient care and revenue cycles
RPA bots connect directly to EHR/EMR platforms, billing systems, patient portals, and lab information systems — without replacing them. UiPath, for instance, has expanded professional services specifically for electronic medical records platforms. That expansion reflects a core advantage of RPA: hospitals and health systems protect their existing infrastructure investments while still gaining automation benefits.
That works well for structured, rules-based processes — but healthcare data is rarely clean or consistent. That's where the next evolution comes in.
From RPA to Intelligent Process Automation
Basic RPA handles structured data and follows predefined rules. Intelligent Process Automation (IPA) extends this by incorporating AI subdisciplines like machine learning, natural language processing, and computer vision. This enables bots to:
- Interpret handwritten physician notes
- Extract data from scanned insurance documents
- Make judgment-based decisions on unstructured inputs
- Flag anomalous billing patterns through adaptive pattern recognition
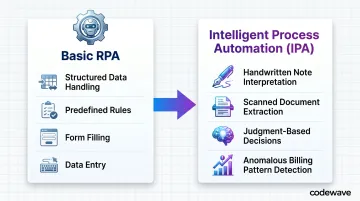
Research shows that integrating AI with RPA in healthcare enhances decision-making quality and workflow efficiency — a shift that moves automation from task execution into genuine clinical and operational decision support.
Top RPA Use Cases in Healthcare
RPA delivers the most value when deployed against high-volume, rule-driven, error-prone processes. Below are the most impactful use cases currently transforming healthcare operations.
Appointment Scheduling and Patient Onboarding
Bots handle the full scheduling cycle:
- Process incoming patient requests from phone, web, and portal channels
- Check real-time physician availability and match with patient needs
- Book or reschedule appointments automatically
- Send confirmation and reminder messages via SMS, email, or app notifications
- Collect demographic, insurance, and medical history data from intake forms
- Populate EHR systems with onboarding information
Impact: Reduces manual call center workload, eliminates scheduling errors, decreases no-show rates through timely reminders, and accelerates patient onboarding.
Claims Processing and Medical Billing
Claims processing remains one of the most labor-intensive and error-prone administrative workflows in healthcare. According to the CAQH Index, $89 billion is spent annually conducting administrative transactions, with $18.3 billion in potential savings through full electronic adoption.
What bots automate:
- Aggregating patient treatment and diagnosis data from EHR systems
- Populating claim forms with CPT codes, ICD-10 codes, and patient identifiers
- Flagging missing or non-compliant information before submission
- Submitting claims to insurers electronically
- Tracking approval status and payment timelines
- Routing rejected or denied claims to human reviewers with context
Documented outcomes:
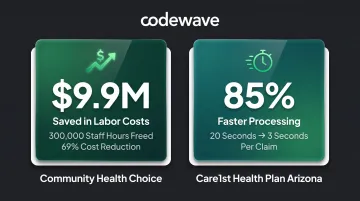
- Community Health Choice saved $9.9 million in labor costs and freed 300,000 staff hours, achieving a 69% cost reduction
- Care1st Health Plan Arizona reduced claim processing time from 20 seconds to 3 seconds per claim
EHR and Patient Data Management
Healthcare providers struggle with fragmented patient data across multiple systems. Manual data entry introduces errors that compromise care quality and regulatory compliance.
Automation scope:
- Extracting and migrating patient records between disparate EHR platforms
- Reconciling duplicate entries and flagging data inconsistencies for review
- Auto-populating structured fields from unstructured intake documents and clinical notes
- Syncing lab results, imaging reports, and medication histories across systems in real time
- Generating audit-ready data logs to support HIPAA compliance workflows


